Skipping a bone graft before implants can cost you more than money; it can lead to implant failure, shifting teeth, and extra surgeries. If your jaw lacks enough bone, placing an implant without a graft greatly raises the risk the implant will not fuse and will fail.
You should know what to expect: grafting adds time and expense up front, but it often prevents bigger problems later. Understanding options, recovery time, and likely costs helps you avoid surprise treatments and repeated procedures.
Key Takeaways
- Missing a graft increases the chance of implant failure and extra surgeries.
- Investing in bone buildup now can prevent larger costs and complications later.
- Learn your options and costs so you can make a clear plan for jaw health.
Why Bone Grafting Matters for Dental Implants
Bone grafting builds the jaw structure implant posts need and prevents future bone loss. It affects how stable your implant will be, how long the implant lasts, and how the final tooth looks.
Role of Bone Grafts in Implant Placement
A bone graft restores missing bone so your dental implant has solid support. Implants need enough jawbone density and volume to hold the titanium post steady during osseointegration. If your ridge is too thin or short, the implant can tilt or fail to integrate.
Surgeons may use autogenous bone (your own bone) or processed graft materials to fill the defect. They place grafts in specific spots (ridge augmentation for width, sinus lifts for upper back teeth) to create the proper shape and height for the implant platform.
A successful graft helps you get the right implant size and angulation. That improves chewing function and makes the crown look natural.
Consequences of Insufficient Bone for Implants
If you skip a needed bone graft, the implant may lack primary stability. That increases the risk of early loosening and implant failure within months.
Insufficient bone also raises problems with implant angulation. Poor angulation can cause chewing issues, stress on surrounding teeth, and a visible metal edge near the gum line. You may need extra surgery later, such as corrective grafting or implant removal.
Long-term, untreated bone resorption after tooth loss can change your facial profile and make future restorations harder. Fixing that later usually costs more and takes longer.
How Bone Grafting Stimulates New Bone Growth
Graft materials act as a scaffold where new bone cells grow and blood vessels form. Over months, the graft integrates and becomes living bone that can bond with the implant surface.
Different graft types work in different ways: autogenous bone adds living cells and growth factors; allografts and xenografts provide a safe scaffold; synthetic grafts offer predictable structure. Your surgeon picks the option that matches your defect and health.
Care after surgery (good oral hygiene, avoiding smoking, and following instructions) helps blood supply and cell activity so the graft matures on schedule for implant placement. Consider imaging like CBCT to track graft volume before the implant is placed.
Potential Complications of Skipping a Bone Graft
Skipping a bone graft can make implants less stable, raise the chance they will fail, and lead to more surgeries later. It can also speed jawbone loss and change how your face looks over time.
Implant Failure and Instability
If your jaw lacks enough bone volume, the implant may not anchor properly. That weak support increases the risk the implant will wobble, loosen, or fail to fuse with your bone (osseointegration).
A loose implant can cause pain, infection, or movement when you chew. You may lose the implant and the abutment, and need removal. Replacing a failed implant often costs more and takes longer than doing a graft first.
To reduce these risks, clinicians evaluate bone with 3D imaging. If the scan shows thin or soft bone, a jaw bone graft is commonly recommended to give the implant a secure foundation.
Accelerated Bone Loss and Jawbone Resorption
An implant needs bone stimulation to stay stable. Without enough bone, the surrounding jaw can continue to resorb (shrink). That bone loss can widen over months or years.
When bone resorbs, nearby teeth can shift and future implant sites become harder to treat. You may lose vertical height in the jaw, which makes later grafts more complex. Missing a graft now often increases the chance you’ll need larger grafts later to prevent further bone loss.
If you want to prevent bone loss, a bone graft at the right time helps preserve volume and keeps the implant-supported tooth functioning like a natural root.
Need for Additional Oral Surgery
Avoiding a graft now can lead to more operations later. You might need larger bone grafts, sinus lifts, or ridge augmentation to rebuild lost bone before a new implant can be placed.
Research has found that bone augmentation techniques, when improperly planned or executed, can be a significant risk factor for early implant failure, with some contexts showing an odds ratio above 9.
Each extra surgery brings more cost, longer healing, and higher risk of complications like infection or graft failure. You could face a staged approach: graft first, wait months for healing, then place the implant. That extends treatment time and adds appointments.
Choosing a timely jaw bone graft can often minimize the number and scale of future oral surgeries and lower the total cost and downtime.
Impact on Facial Structure and Aesthetics
When jawbone resorbs, your facial profile can change. Loss of bone under the cheeks or lips can cause a sunken look, thinner lips, and deeper wrinkles around the mouth.
If you skip a bone graft and implants fail or sit poorly, crowns may look uneven or unnatural. Restoring that appearance later often needs both grafting and more complex prosthetic work.
A well-placed graft helps keep your bone height and contours. That supports both the implant and the soft tissues that shape your face, helping maintain a more natural appearance.
Types of Bone Grafts and Alternatives
You need to know the main graft materials, when extra surgery like a sinus lift or ridge augmentation is needed, and what non-graft options may let you get implants faster or with less risk.
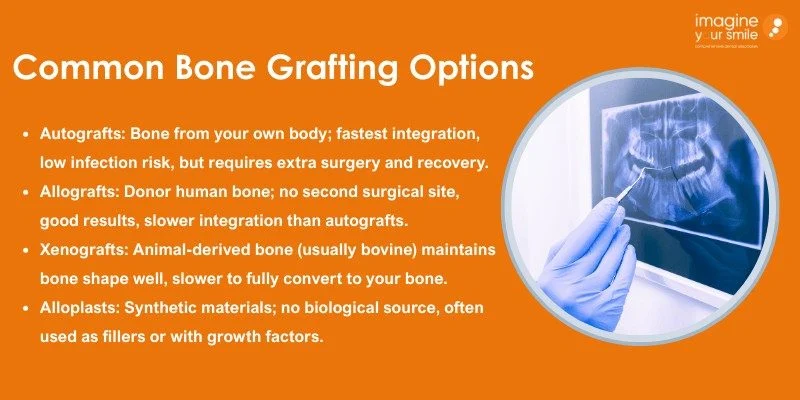
Autografts, Allografts, Xenografts, and Alloplast
Autografts use bone taken from your own body, often the chin or hip. They integrate fastest and lower infection risk, but require a second surgical site and longer recovery.
Allografts come from human donors and are processed to be safe. They avoid a second wound and work well for many defects, though they can take longer to fully integrate than autografts.
Xenografts use animal-derived mineral scaffolds, commonly bovine. They hold shape well and help maintain ridge volume, but they may resorb more slowly and sometimes leave mineral that never fully converts to your bone.
Alloplasts are synthetic materials like calcium phosphate. They are plentiful and avoid biological sourcing. Many are used as fillers or combined with biologics to boost bone growth.
Key decision points for you: defect size, desire to avoid donor sites, and how quickly you need an implant. Talk with your clinician about trade-offs for integration time, donor-site pain, and long-term volume stability.
When Sinus Lift and Ridge Augmentation Are Needed
A sinus lift raises the sinus floor and adds bone to the upper back jaw when there isn’t enough height for implants. You may need this if your upper molars were lost long ago or your sinuses sit low. The surgeon places graft material under the lifted membrane and waits several months for new bone to form.
Ridge augmentation rebuilds width or height of the jaw where bone has shrunk after tooth loss. Small defects may use particulate grafts and membranes; larger defects often need a block bone graft secured with screws. Blocks can come from your own bone (autograft) or donor bone (allograft).
Both procedures increase implant success by creating a stable foundation. They add time and cost, and healing typically takes 3–9 months depending on the graft type and location.
Alternatives to Bone Grafting for Implants
If you want to avoid grafting, some implant methods work around low bone. Zygomatic implants anchor into the cheekbone for the upper jaw when the back jaw lacks bone. The All-on-4 approach angles implants to use denser front bone and often avoids grafts for full-arch restorations.
Short or narrow implants fit into limited bone but require careful planning and may not suit all bite forces. In some cases, immediate placement with socket preservation limits bone loss and reduces the need for later grafting.
Each alternative has limits: they change implant angles, need specific bone quality, or can raise surgical complexity. Compare long-term stability, cost, and how soon you need teeth with your dentist before choosing an alternative.
Financial Implications: The True Cost of Skipping a Bone Graft
Skipping a needed bone graft can lower your bill today but often raises it later. You may face implant failures, extra surgeries, and surprise fees that add up faster than the initial graft cost.
Additional Expenses from Implant Complications
If your jaw lacks enough bone, implants can fail or loosen. You may then need removal of the failed implant, which adds surgeon fees and anesthesia costs. Each removal visit can cost several hundred to a few thousand dollars depending on your location and provider.
Failed implants also increase the risk of infection. Treating an infection may require antibiotics, extra office visits, and sometimes minor surgery to clean the area. Those bills are rarely included in your original implant quote.
You might also pay more for temporary solutions. If an implant fails, you may need a removable denture while you heal. Temporary prosthetics, adjustments, and extra lab work can add up to several hundred dollars per month.
Cost of Complex Revision Treatments
When bone loss progresses, your corrective options get more complex and costly. A block bone graft or a sinus lift for the upper jaw often costs significantly more than a small socket graft. Complex bone grafting can range from a few thousand to over five thousand dollars depending on graft type and surgeon experience.
Revision implant surgery often includes multiple staged procedures: grafting, months of healing, then new implant placement. That means repeated surgical fees, CT scans, and longer overall treatment time. Each stage can carry its own surgical and anesthesia costs.
Specialist care also raises prices. Oral surgeons or periodontists who handle complex revisions command higher fees than general dentists. If your original plan used bundled pricing, revisions may fall outside that bundle and become separate, uninsured charges.
Hidden Fees and Price Breakdown
Initial quotes for implants sometimes list implant surgery but exclude grafting, scans, lab fees, and follow-up visits. Ask for a line-by-line cost estimate so you can compare graft cost versus downstream expenses. A simple breakdown should show: graft material cost, surgical fee, anesthesia, imaging (CBCT), and lab/prosthetic fees.
Graft material affects price. Autografts (your own bone) add harvesting fees. Allografts (donor bone) and synthetic materials have different price points. A block bone graft typically costs more than particulate grafts because of added surgery time and harvesting needs.
Look for bundling and financing options. Some clinics offer bundled pricing that includes grafting, implant, and restoration for one fee. If you don’t get a bundle, ask about payment plans or third‑party financing to spread costs.
Transparent billing helps you weigh the upfront bone graft cost against likely revision and complication expenses.
Making Informed Decisions: Diagnosis, Insurance, and Payment Options
You need clear facts about how your dentist checks bone, what parts insurance may cover, and payment choices if you need a bone graft. Know the tests, likely costs, and the practical steps to get treatment without surprises.
How Dentists Diagnose Bone Loss for Implants
Your dentist starts with a clinical exam and history about missing teeth or past extractions. They will check gum health, tooth spacing, and signs of bone shrinkage by touch and visual inspection.
Imaging follows. A periapical or panoramic X-ray shows general bone height. For precise planning, your dentist will order a cone beam CT scan to measure bone width, density, and the exact shape of the ridge.
Those measures tell whether you need a socket preservation graft after extraction or a larger bone graft before implants.
Expect discussion of alternatives: mini implants if bone is thin, or staged treatment where a graft heals 3–9 months before placing implants. Ask for images and measurements so you understand why a graft is recommended.
Insurance Coverage and Reimbursement
Dental plans vary widely. Basic dental insurance often covers tooth extraction but rarely pays full cost for bone grafting tied to implants. Medical insurance sometimes helps if bone loss follows trauma or disease, but you must check policy rules.
Document everything. Get a written treatment plan, procedure codes, and a pre-treatment estimate from your dentist. Submit these to your insurer before surgery. Common CPT/ADA codes for grafts and extractions matter for claims. If a claim is denied, ask for an itemized denial and appeal with supporting X-rays or a specialist letter.
Keep receipts and note dates. Some flexible spending accounts (FSA) and health savings accounts (HSA) can reimburse grafts. Verify whether socket preservation grafts after an extraction get different coverage than augmentation solely for implants.
Financing and Payment Plans for Bone Grafting
If insurance doesn’t cover the graft, ask about in-office financing and third-party plans. Many practices offer 3–12 month no-interest plans or extended low-interest loans that break the cost into monthly payments.
Compare the total cost, not just monthly amount. Look for fees, down payments, and penalties for missed payments. Credit options include medical credit cards and personal loans; compare APR and term length.
Ask the office for a payment worksheet that lists: surgical fee, graft material (autograft vs. donor vs. synthetic), CT scan, anesthesia, and follow-up visits. That helps you plan for added costs like socket preservation at extraction or a separate graft surgery before the implant.
Long-Term Benefits of Addressing Bone Loss Before Implant Surgery
Addressing jawbone loss before getting implants gives you a stronger base, lowers implant failure risk, and keeps your bite working well for years. Fixing bone issues first also makes future care simpler and protects the look of your face.

Improving Implant Stability and Success Rates
When you add bone with a graft, you increase the surface area that the implant can fuse to. That fusion, called osseointegration, is how the implant becomes stable. With more bone volume, your implant is less likely to loosen or fail during the first year after surgery.
Studies show dental implants generally have a 97% survival rate at 5 years and 90% at 10 years, but this depends heavily on adequate bone to support osseointegration
Bone grafts can use your own bone or safe substitutes to stimulate new bone growth around the implant site. This helps implants handle chewing forces right away and reduces tiny movements that can block healing. Strong early stability also lowers the chance you’ll need corrective surgeries later.
Protecting Oral Health and Function
A solid bone foundation helps implants support crowns and bridges without shifting. That keeps your chewing function normal so you can eat a variety of foods without pain. Stable implants also protect nearby teeth by sharing bite forces correctly.
Treating bone loss lowers infection risk because well-integrated implants seal better against bacteria. Good bone levels make cleaning around implants easier, too, which cuts the chance of gum disease that can damage both implants and natural teeth.
Preserving Jawbone Structure for the Future
Bone grafting restores height and width to the jaw so your face keeps its natural shape. Preserving the alveolar ridge prevents the sunken look that can follow long-term tooth loss. That matters if you want implants or other dental work years from now.
By preventing further bone loss, you keep options open: future implants, fixed bridges, or denture support become easier and less costly. Early bone regeneration reduces the need for larger, more complex oral surgery later, saving you time and lowering surgical risk.
Frequently Asked Questions
This section answers cost (and cost-related) questions you are likely to face when a bone graft is part of implant care. It covers how insurance, graft type, number of implants, location, and typical price ranges for a molar graft affect your out-of-pocket spending.
How can insurance impact the overall costs of a bone graft?
Insurance can cut your bill if your plan covers part of the procedure or related services like extractions or imaging. Some dental plans classify grafting as reconstructive or medically necessary, which raises your chances of coverage.
You may still face deductibles, co-pays, or annual limits that leave several hundred to several thousand dollars for you to pay. Ask your insurer for a pre-authorization and a written estimate so you know what they will pay and what you must cover.
What factors influence the cost of a bone graft for a single tooth?
Graft material matters: autografts (your bone) usually cost more due to added surgery time; allografts or xenografts cost less. The graft size and complexity (ridge augmentation, sinus lift, or socket preservation) also change the price.
Your provider’s fees, imaging (like CBCT), sedation choice, and whether you need an extraction or membrane add to the total.
Clinic location and the surgeon’s experience can push costs higher or lower.
What are the financial implications of getting two dental implants with bone grafting?
Costs roughly double for two implants, but some fees (imaging, consultations) are shared and may not be fully duplicated. Each implant adds implant hardware, abutments, and crowns, plus any graft material needed at each site.
Plan for a combined cost that includes grafting at each implant site, separate surgical visits if staged, and two final crowns.
Ask your clinic for an itemized quote that lists graft materials, implant components, and lab work.
Is it possible to avoid a bone graft before implants and what are the consequences?
You may avoid grafting if you already have enough bone height and width for the implant.
Less invasive options include using shorter or narrower implants, or angled implants placed by a specialist.
Skipping a needed graft risks poor implant stability, higher failure rates, and more expensive repairs later.
Discuss long-term outcomes with your surgeon before choosing to skip grafting.
How do different locations, such as California, affect the cost of bone grafting?
High-cost areas like California often charge more for surgery, facility use, and staff time, increasing your bill. Urban clinics and specialized surgical centers usually cost more than rural or general dental offices.
Regional demand and local cost of living influence fees for graft materials and surgeon rates. Compare quotes from multiple practices in your area to see typical local pricing.
What is the average cost of a molar bone graft without dental insurance?
A single molar bone graft commonly ranges from about $500 to $5,000 depending on graft type and complexity. Simple socket preservation sits at the low end; larger ridge or sinus procedures sit at the high end.
Ask for a written estimate that shows graft material, surgical fees, and follow-up care so you can compare prices clearly.
For local averages and planning, check clinics near you and request cost breakdowns before scheduling.